
Dorothy Hodgkin won the Nobel Prize in Chemistry for showing vitamin B12’s three dimensional structure.
Vitamin B12 history in brief
1850s — English doctor, Thomas Addison, described a lethal “pernicious” form of anemia, related to pathological gastric mucosa. In other words, a destructive but gradual form of anemia appeared when the stomach lining became diseased. He showed that the anemia was associated with the stomach having little or no acid once its lining became diseased.
1926 — Georges Richard Minot and William Parry Murphy reported that 45 patients with pernicious anemia had been cured by eating large quantities of raw liver.
1929 — William Castle discovered that “intrinsic factor” was needed in the stomach in order to absorb extrinsic factor, later known as vitamin B12. He discovered that intrinsic factor was lacking in pernicious anemia patients.
1934 — Minot, Murphy and Whipple received the Nobel Prize in Medicine for their research isolating extrinsic factor and identifying it as a vitamin. Vitamin B12, to be exact.
1948 — Pure vitamin B12 was produced.
1956 — British chemist, Dorothy Hodgkin, described the structure of the vitamin B12 molecule.
1964 — Dorothy Hodgkin received the Nobel Prize for Chemistry.
Pernicious Anemia was fatal
Before there was any known cure, pernicious anemia was fatal. It was like cancer.
Turning points came when intrinsic factor was discovered, followed by the identification of vitamin B12. Prior to that, the discovery that people with pernicious anemia could be cured by eating quantities of raw liver was a huge step forward. Except, raw liver was a rather unpalatable cure. Today, the list of vitamin B12 foods is rich and appetizing.
Production of vitamin B12 was a dramatic leap forwar,d, and soon after came the discovery that pernicious anemia patients recovered when given injections of vitamin B12, as cyanocobalamin.
Perhaps not surprisingly, the early identification of anemia linked to vitamin B12 deficiency presents a lingering problem. Once it was known that blood cells in B12 deficient people were larger than normal, that became the gold-standard symptom in identifying B12 deficiency.
The fact B12 deficiency was known to be accompanied by nerve/neuropsychiatric problems was entirely overshadowed by the blood disorder, anemia. The belief was that without large blood cells, there was no B12 deficiency.
This inaccurate belief is being whittled away as new “markers” for vitamin B12 deficiency are found. Two markers relating to intracellular functional B12 deficiency are methylmalonic acid and homocysteine.
Pernicious anemia with its lack of intrinsic factor is now thought to be relatively rare. In fact, today it has become clear that anemia is only one of many different signs of low vitamin B12 levels.
47% of Americans have Hypochlorhydria?
Hypochlorhydria, less familiar than pernicious anemia, is the condition of insufficient stomach acid to separate vitamin B12 from food.
An estimated 47% of people in the U.S. have hypochlorhydria, partially due to increased use of antacids marketed as a good source of calcium.
Research shows that smoking, high alcohol consumption, NSAIDS like Ibuprofen, and many prescription drugs reduce B12, as do some common genetic polymorphisms (variations occurring within a species) that affect enzyme activity.
Personally, I think the underlying problem reducing B12 is high stress. I wonder if people smoke and drink to relieve stress because they can feel the damage stress is doing. I’m not saying drinking and smoking are a cure for problems arising from stress; I’m saying it’s very possible that when stress is lowered and/or B12 levels are increased there is less desire to smoke and drink, on a purely physical level.
Functional B12 Deficiency
Scientific testing over a long period showed “functional deficiency,” that is, an insufficient distribution of B12 at the cellular level, could come about even though serum levels were normal.
This is extremely important to know and understand. It explains why people experience problems related to low vitamin B12 levels, go to their doctor, get a B12 test, and subsequently are told their B12 is “fine.”
![]() Vitamin B12 lozenges help you have healthy nerves and blood.
Vitamin B12 lozenges help you have healthy nerves and blood.
Sadly, the American medical community sees fit to keep the “normal” range extremely low, which fosters confusion, mis-diagnosis, and higher pharma profits.
News reports during 2008 linked doctor prescriptions with kick backs from drug companies, making the medical community’s favoritism for drugs over nutrients less sad and more criminal. But… nearly imposible to prosecute.
With that being the reality, it’s important to look at a comprehensive list of signs of low vitamin B12 levels; if some pertain to you, buy Methylcobalamin lozenges, which you dissolve under your tongue, and begin using them… AND begin keeping a time line of your experience… what symptoms are you feeling? are symptoms strong? do they grown less strong? what stress are you under? and, keep track of the lozenges you use, their strength as well as the number you use. (A 1,000 mcg Methycobalamin lozenge a day, every day for a month, is equal to a B12 shot. Using two a day would equal a shot in 15 days, half a month. Basically, more works faster. As healing takes place in red blood cells, however, you could experience painful muscle contractions due to insuficient potassium in your system to handle the red blood cell activity when there’s enough B12. Potassium is very easy to get from food. There’s a list of potassium foods on the potassium page.)
Illustrations
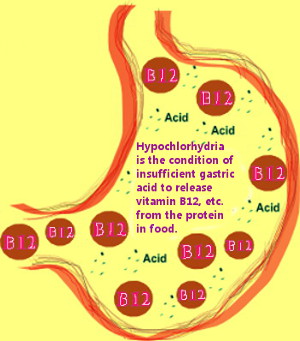
Too little stomach acid results in vitamin B12 remaining trapped in protein. Warning signs of low gastric acid can be found half way down the linked page.
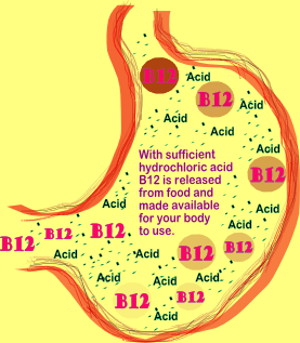
When there is adequate stomach acid vitamin B12 is released from protein.
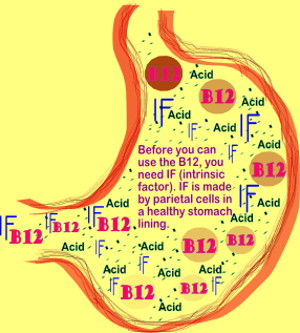
You need intrinsic factor before vitamin B12 in food can be used by your body. Methylcobalamin lozenges do not require intrinsic factor.
Amazing microscopic view of B12.
While expensive tests are developed to test for B12 deficiency, for example using a determination of holotranscobalamin, the transport protein with selectively bound active cobalamin . . . Learning to recognize signs of low B12 in your body is your BEST DEFENSE against the ravages of B12 Malabsorption and low vitamin B12 levels:
Your fingernails reveal your B12 health
